
Luckily, we are highly skilled in treating a variety of conditions and issues. Whether you have slight discomfort or severe pain, we can provide you with care that allows you to live the lifestyle you want!
These are just some of the conditions, treatments, and services you will find at our podiatric office. Just ask us if you have any questions!
- Custom Orthotics
- Digital XRays
- Sports Medicine
- Surgical Corrections of Foot Disorders
- Wound Care
- Achilles Ruptures
- Arthritic Foot Care
- Cavus Foot
- Chronic Wounds Treatment
- Congenital Deformities
- Diabetic Limb Salvage
- Hallux Rigidus
- Lisfranc Injuries
- Minimally Invasive Surgery
- Osteochondral Lesion of Talus
- ESWT
- Lapiplasty® 3D Bunion Correction

Custom Orthotics
Foot orthotics are medical devices that a podiatrist will prescribe to treat a patient’s specific foot condition or to correct a biomechanical issue or gait anomaly. These types of orthotics are custom fitted, designed, and created, based on the patient’s actual foot and medical needs, and worn in the patient’s footwear.
What Conditions Can Orthotics Treat?
Custom orthotics can treat a variety of painful foot conditions and mobility issues including:
• Plantar fasciitis
• Arthritis
• Bursitis
• Heel spurs
• Bunions
• Flat feet
• High arches
• Improper foot alignment
• Gait disorders caused by pronation or supination issues
• Balance issues
How Are Custom Orthotics Made?
Prescription orthotics are customized to each patient’s feet. Either a plaster mold or a 3D digital scan will provide a model of the patient’s actual foot. Following the podiatrist’s prescription, the orthotic will be constructed with specific long-lasting, high-quality materials that achieve different objectives.
Rigid Orthotics. Rigid, or functional orthotics are typically made from firm materials such as carbon fiber or plastic. These types of orthotics are designed to control motion and joint function. They can be used to treat muscle strain, foot pain, flat feet, Achilles tendonitis, sesamoiditis, and pain in the lower back, legs, and thighs.
Soft or accommodative orthotics. These devices are made of softer, more flexible materials such as EVA foam or gel. They are designed to offload pressure and cushion sore or uncomfortable areas of the feet. They can help prevent and treat conditions such as diabetic foot ulcers, plantar fasciitis, and more.
Semi-rigid orthotics. These combine the control of a rigid orthotic with the cushioning features of a soft orthotic. They use softer material which has been reinforced by more rigid materials. These types of orthotics are often used to help provide balance when walking or doing sports, or to treat flat feet or gait abnormalities in children learning to walk.
Talk to your podiatrist about custom orthotics to explore whether they can help treat your pain or correct your alignment or gait issue.

Digital X-Rays
At Harlis Family Foot and Ankle, we value your time and are proud to offer our patients in-house, state-of-the-art digital radiographs. We understand that proper treatment begins with an accurate diagnosis, and our digital x-ray service enables us to diagnose and confirm any bone or soft tissue injuries and conditions that can be hard to determine through a physical exam. Unlike traditional x-rays that use film, digital x-rays are safer exposing patients to less radiation and faster allowing doctors to view results within minutes. With this state-of-the-art technology, we can save you time and begin customizing treatment and therapies for your needs.

Sports Medicine
We know how much your foot health can impact your athletic performance, and it is our priority to help get you off of the sidelines and back in the game. Whether you are dealing with a recurring injury or an accident from the big game, we are here to support you through each step of your therapy. Below is a list of some of the most common sports and sports-related injuries we see in our office:
- Martial Arts and Kickboxing: Plantar fasciitis, Achilles tendonitis, sesamoiditis, and ankle sprains. Proper stretching is vital to injury prevention, specifically, a minimum of 15 minutes before beginning exercise.
- Aerobics: With 26 bones in the foot and impact forces reaching up to six times the force of gravity, proper shoes are essential when participating in aerobics. Shoes must provide shock absorption and proper cushioning, as well as stability.
- Team Sports: Baseball, basketball, soccer, football, field hockey, and lacrosse often lead to foot and ankle injuries. Artificial surfaces, improper footwear, and inadequate stretching are recipes for disaster.
Surgical Corrections of Foot Disorders
In most cases, invasive methods are not necessary to correct many foot disorders. Though in more extreme conditions, surgery may be required. The need for surgery will depend on the severity of the condition, the amount of pain the patient is experiencing, and the patient’s past response to various treatments.
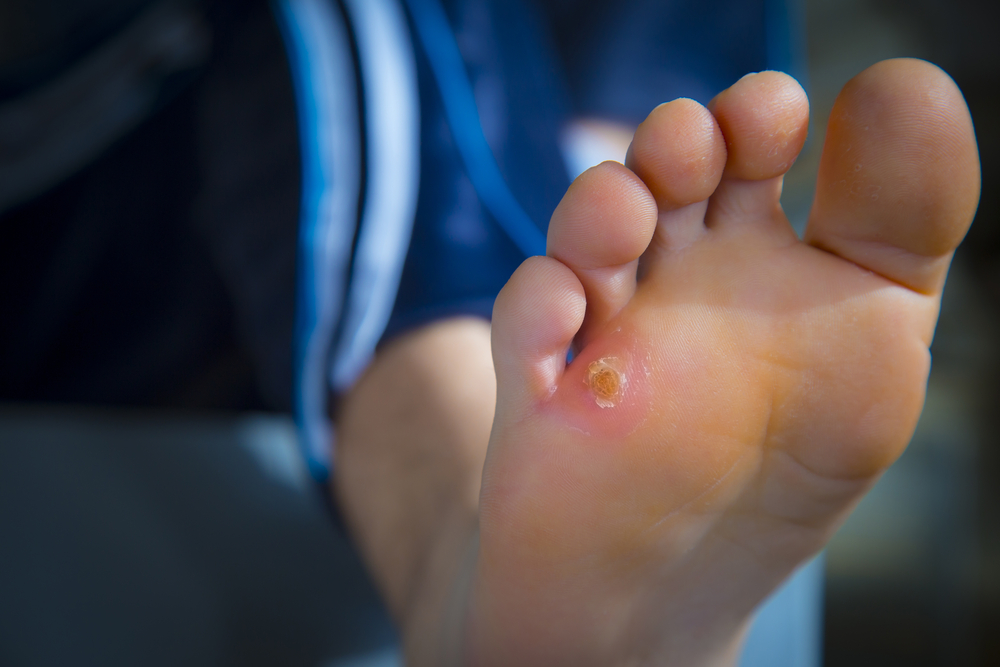
Wound Care
Ulcers on the foot may not always come with pain, but they are serious conditions that should be evaluated by a medical professional. The symptoms of ulcers may include drainage, or red, inflamed tissue. To properly diagnose and develop a treatment plan x-rays may be ordered.

Achilles Ruptures
Achilles tendon rupture is a serious issue that affects normal ambulation. It usually happens in individuals playing sports, yet it can happen to anybody. Achilles tendon rupture leads to Achilles tendon pain. That pain may be hard to bear. So it is very important to get treatment for the Achilles tendon injury or sore Achilles tendon. Our team of capable doctors and surgeons at Harlis Family Foot and Ankle located in Port St. Lucie, Florida can address your problem. They are also more than capable in handling Achilles tendonitis treatment in Port St. Lucie.
The Achilles ligament is a solid tendon that connects the muscles toward the rear of your calf to your heel bone. Assuming you overstretch your Achilles ligament, it can completely tear or partially tear the tendon causing Achilles tendon pain.
Assuming your Achilles tendon rupture, you may hear a pop, trailed by a prompt sharp discomfort toward the rear of your lower leg. Usually, parents find it difficult to walk appropriately. Surgical procedures are frequently performed to fix the tear. For some individuals, be that as it may, nonsurgical treatment works similarly as well.
Causes of Achilles Ruptures and sore Achilles tendon:
Factors that might increase the risk of Achilles Rupture include:
- Age. The pinnacle age for Achilles ligament break is 30 to 40.
- Sporting games.
- Steroid injections.
- Certain antibiotics. Fluoroquinolones like ciprofloxacin (Cipro) or levofloxacin (Levaquin), increase the danger of Achilles ligament crack.
- Weight.
All these causes are individually discussed with each individual at our medical facility in Port St. Lucie.
How to avoid the Achilles Rupture:
- Stretch before increased activity
- The balance between high impact sports and low-intensity activities.
- Run-on even surfaces
- Dress appropriately for the activity/sporting event
- Gradually increase activity level.
Achilles tendonitis treatment:
There are several methods for achilles tendonitis treatment. These treatment methods include NSAIDS, immobilization, platelet-rich plasma (PRP) infusions, and surgical procedures. If you find yourself with achilles tendon pain or if you may have suffered an achilles tendon tear, give us a call at Harlis Family Foot and Ankle, where one of our specialized physicians can treat you.

Arthritic Foot Care
Ankle arthritis is a form of inflammation which is caused from ankle cartilage injury. This could be from a ankle fracture, bad ankle sprain or recurrent ankle sprains/rolling of the ankles. The post traumatic ankle osteoarthritis is generated following severe injury. Sometimes, if left untreated, the injury develops the post traumatic arthritis permanently. So it is quite essential to consult your doctor and take the proper treatment. There are in excess of 100 types of joint inflammation, large numbers of which influence the foot and lower leg. Ankle arthritis can make it hard to walk and perform exercises you appreciate. As the issue of arthritis is serious as it can cause much pain and suffering for you, so consult your doctor for the treatment. We have the best physicians at Harlis Family Foot and Ankle in Port Saint Lucie who can treat your issues effectively.
What is Arthritis?
Arthritis is a painful and sometimes crippling disease that afflicts millions of people. It causes swelling and inflammation in the lining and cartilage in joints.
Each foot and ankle has a total of 33 joints. This fact, along with having to bear the body’s weight, make feet and ankles more susceptible to arthritis and its painful, often debilitating symptoms.
What Causes Arthritis?
Arthritis can be caused by a number of factors including:
• Genes which predispose a person to arthritis
• Injuries that cause joint damage
• Old age which causes joints to get worn down
• Infections in joints that are viral, bacterial, or fungal
• Excess Weight that puts extra wear and tear on joints
• Jobs requiring repetitive movements or lifting heavy objects
Types of Arthritis and Their Symptoms
Osteoarthritis. The most common type of arthritis, osteoarthritis causes a degradation in the cartilage on the ends of bones, causing them to rub against each other. Symptoms may include joint pain, tenderness and swelling, a grating sensation, bone spurs, joint deformity and decreased mobility.
Rheumatoid arthritis. This occurs when the body’s immune system attacks joint linings. Symptoms may include pain, stiffness, swelling, tenderness or warmth in the joints and nearby tissues, fever, loss of appetite and fatigue.
Gout. When there are high levels of uric acid in the blood, needle-like urate crystals can form in joints which may cause flare-ups of severe pain, inflammation and redness in the joints, and a limited range of motion.
Tips For Arthritic Foot Care
Practicing the following arthritic foot and ankle care at home can sometimes help lessen the severity of symptoms like pain and stiffness:
Footwear. Wear shoes that are flexible, supportive, with proper arch support, low heels, cushioned soles, and plenty of room in the toe box.
Custom Orthotics. Custom-made orthotic devices can provide much needed support exactly where you need it, while preventing friction and pressure on sore spots.
Heat and Ice. Ice, creams, and heating pads can sometimes help increase circulation in the affected area, which may reduce symptoms and reduce inflammation.
Medication. Nonsteroidal anti-inflammatory drugs (NSAIDs) may provide some relief, although they are not suitable for long-term use, nor are they a permanent solution to managing the disease.
Since arthritis is a complex disease, a podiatrist can provide professional techniques to ease your suffering and help you combat this painful and often debilitating disease.

Cavus Foot
Pes Cavus is the medical term that describes a person with high arched feet. It is not as common as pes planus, or flat feet, but can still cause some uncomfortable symptoms such as pain in the arch of the foot.
How to tell if you have high arches?
Evaluating the integrity of your foot arches is generally done standing up. So if your arches look high when sitting down, but fall when you stand up, you actually don’t have high arches. X-rays and other diagnostic testing performed by a podiatrist can also determine if you have high arches.
What are some symptoms of high arches?
High arched foot problems can appear with a wide range of symptoms and sequela such as arch pain in the foot, hammertoes, muscular spasms, and severe callous formation at the front of the foot. Luckily, there are many surgical and non-surgical treatment options for high arched feet that our doctors at Harlis Family Foot and Ankle specialize in.
What are some treatments for high arched feet?
Depending on symptoms, one of the best and most effective treatments is to use shoes for high arches. These include shoes with extra cushion, and sometimes extra depth. The cushion will help with shock absorption, especially if you have pain in the heels or under the metatarsal heads. Some doctors also advocate a high topped shoe to protect the lateral ankle ligaments. If conservative treatment measures don’t help, there are a wide range of surgical procedures that can be performed to make the foot more functional.
If you find yourself suffering from painful high arches and need to discuss your treatment options, please call Harlis Family Foot and Ankle, and schedule an appointment with one of our qualified physicians today!

Chronic Wounds Treatment
There are 4 stages of wound healing. Hemostasis, inflammatory, proliferative and maturation. For wounds to heal they must go through all 4 stages. Chronic wounds are wounds that are stuck in one stage of wound healing, which is usually the inflammatory phase. There are a number of reasons why a wound may get stuck in this stage of healing including but not limited to pre-existing conditions such as diabetes, peripheral vascular disease, malnutrition, and being immunocompromised.
It is important to know that some wounds or ulcers may simply need 1-2 modifications to jump-start healing, however, in the face of pre-existing conditions wounds may take a lot longer to heal sometimes 6 months to a year. However, it is extremely important that you are following up with a physician during this time period because open wounds can become infected quickly and a specialist, like our doctors at Harlis Family Foot and Ankle, will know what needs to be done to move past the infection and get you back on track.
A wound may start off as a simple leg cut, or multiple leg wounds. Unfortunately, as time passes and that wound is not healing on your lower leg or foot, it can progress to a non-healing foot wound or non-healing leg wound. To address how to get the wound to heal we must take a deep look at why this wound is stuck in its current stage. Our doctors obtain a thorough history and physical and run a number of tests to assess blood flow, nutritional status, as well as identifying any medical history that can also be contributing to impeding healing. Our physicians at Harlis Family Foot and Ankle in Port St. Lucie are well trained and available to treat your chronic wounds.
Some of the treatment modalities that we use to treat non-healing foot wounds and non-healing leg wounds are:
- Serial debridements
- local wound care
- Home health care with one of our trusted Home health care agencies
- Advanced wound care modalities such as allografts and wound vacs
If you find yourself with a wound on the ankle not healing, non-healing foot wounds and non-healing leg wound you should seek the consultation of a physician immediately.

Congenital Deformities
Apparent deformities in the body that are produced at or before birth are called congenital deformities. These are also genetic birth defects. These disfigurements might influence the facial construction, for example, with congenital fissure, or might be skeletal, for example, with clubfeet or spina bifida. A child might be feeling the loss of an appendage or have one more limited than the other, or may have an additional toe or finger. The most severe birth defects (some of the time alluded to as birth abandons) incorporate neural cylinder absconds, heart surrenders, and Down disorder, a long-lasting condition that might cause extra medical issues for the kid.
Babies birth defects are unusual things about your infant baby’s body. Each four and a half minutes, a child in the United States is brought into the world with a birth deformity. Genetic disorders in babies and newborns can be:
- Noticeably self-evident, similar to a missing arm or a pigmentation.
- Inner (inside the body), like a kidney that has not framed right or a ventricular septal imperfection (an opening between the lower offices of your baby’s heart).
- A substance awkwardness
- Your child can be brought into the world with one birth imperfection like a congenital fissure (a hole in their upper lip) or various birth deformities like a congenital fissure and congenital fissure (an opening in the top of their mouth) together, or even a congenital fissure and congenital fissure with imperfections of the cerebrum, heart and kidneys.
Your medical services supplier will not have the option to identify all birth defects right when your child is conceived. A few deformities, like scoliosis, probably won’t be obvious until your youngster is a while old. An unusual kidney may require a long time to be found.
Causes of birth defects:
When do most birth defects occur? Natural elements can build the danger of premature delivery, birth deformities, or they may have no impact on your child by any means, contingent upon when during the pregnancy.
Your born child goes through two significant phases of improvement after origination. The first, or incipient organism stage, happens during the initial 10 weeks after origination. A large portion of the significant body frameworks and organs structure during this time. The second, or fetal stage, is the rest of the pregnancy. This fetal period is a period of development of the organs and of the baby overall. Your conceived child is generally helpless against injury during the incipient organism stage when organs are created. For sure, contaminations and medications can cause the best harm when openness happens two to 10 weeks after origination.
Diabetes and overweight might conceivably build your child’s hazard of birth. Our medical specialist at Port St Lucie recommends that you put forth a valiant effort to deal with these conditions before you get pregnant.
A few medications and sporting medications can cause birth defects, which are most serious when utilized during the initial three months of pregnancy. Thalidomide, an enemy of queasiness medication endorsed during the 1960s, caused birth deformities called phocomelia (nonattendance of the majority of the arm with the hands expanding flipper-like from the shoulders).
There is, likewise, isotretinoin, recently known as Accutane or Roaccutane. Isotretinoin is a retinoid, a man-made type of nutrient A that is utilized to treat skin conditions. It causes the fetal retinoid condition. Qualities of fetal retinoid disorder might include:
- Development delay.
- Mutations of the skull and face.
- Irregularities of the focal sensory system.
- Irregularities of the heart.
- Irregularities of the parathyroid organ.
- Irregularities of the renal, thymus organ.
Liquor causes birth defects. Fetal liquor disorder is a term used to portray the commonplace birth defects brought about by the mom’s liquor use:
- Getting handicaps.
- Formative postponement.
- Sensitive to the diseases.
- Helpless coordination.
- Irregularities of facial highlights.
Another natural variable that can cause birth deformities is a uterine requirement. The embryo fills in the mom’s uterus and is encircled by amniotic liquid (like being suspended in a sack of water) that pads it from exorbitant tension. In the event that the sack of filaments that holds the liquid breaks, groups of strands from the torn sack can push on the hatchling and cause amniotic band disorder (which can bring about incomplete constriction of or removal of an arm or leg). An insufficient measure of amniotic liquid can cause extreme strain on the whole child, causing aspiratory hypoplasia (absence of advancement of the lungs).
Clinical science has distinguished the reason for around 30% of birth surrenders. That implies around 70% stay without a direct reason. Upwards of 50-70% of birth deserts are irregular, and their motivation stays obscure. A mix of natural and hereditary elements can build the danger of specific birth abandons.
Preventions of Birth defects:
Can birth defects that are hereditary be prevented? Most birth defects can’t be stopped. There are sure significant stages to advance a sound pregnancy, nonetheless. These tips include:
- See your medical care supplier reliably.
- Assuming you are attempting to consider, or then again in the event that you are physically dynamic and not utilizing contraception, take a pre-birth nutrient with 400 mcg of folic corrosive.
- Contact your medical care supplier quickly assuming that you think you are pregnant.
- Do not drink liquor.
- Do not smoke.
- Converse with your medical care supplier about any drugs and enhancements you are taking.
- Keep away from pot and illicit medications.
For more information, please visit our podiatrist.

Diabetic Limb Salvage
On average, one in every 10 Americans has diabetes. Unfortunately, some of us are predisposed to the condition based upon genetics. Some become diabetic because of unhealthy eating and lifestyle decisions. Thankfully, in this day and age, diabetes is not a death sentence, and diabetic patients can live long and healthy lives!
Regardless, as it pertains to the foot and ankle, diabetic patients are considered at high risk for complications. This is due in large part to neuropathy and the way the disease manifests in small artery disease. Both can have genuine consequences that may create a sequelae for what patients refer to as ‘type 2 diabetes feet’ or ‘type 2 diabetes foot problems’. This is why it is SO important for any diabetic patient to make sure they are seeing a Podiatrist routinely to keep their feet out of harm’s way. Our goal at Harlis Family Foot and Ankle is to prevent complications from diabetes, as much as possible.
Increased times of high sugar levels in the blood can harm numerous spaces of the body, especially the feet.
Diabetes is liable for more than 50% of all foot amputations within the United States. At Harlis Family Foot and Ankle, we have diabetic specialists who will guide you on how to care for your diabetic foot in Port Saint Lucie, Florida.
Symptoms:
Foot manifestations of diabetes fluctuate from one individual to another and may rely upon the particular issues an individual is encountering at that point.
Nonetheless, side effects may include:
- a deficiency of feeling
- ‘deadness’ or shivering sensation
- skin staining and temperature changes
- red streaks
- wounds with or without drainage
In the event that an infection is present, an individual may likewise encounter the following:
- fever
- chills
- high glucose levels
- redness to your foot
Any individual with diabetes who encounters manifestations of an infection, particularly within the feet, should look for Emergent treatment.
Complications of Diabetic Foot:
Diabetic neuropathy and microvascular disease are serious conditions that a specialist should screen intently. :
- foot ulcers or wounds that don’t heal
- infections, including skin diseases, bone diseases, and abscesses
- gangrene
- foot deformation
Some of the time, specialists can prevent or stop infections. Be that as it may, a specialist might suggest amputation if infection or disease is too far spread.
Preventions of Diabetic Foot Complications:
Preventing foot issues is fundamental for individuals who have diabetes. Keeping feet healthy is pivotal, and an individual ought to be watchful with regards to foot cleanliness. They can make the accompanying strides:
- Check the feet every day: Examine the feet day by day, or request that somebody check for any progressions of wounds.
- Wash the feet daily; Keeping the feet clean prevents infections.
- Wear good fitting shoes and socks: Protect the feet in socks and shoes consistently. A podiatrist might prescribe custom shoes to assist with preventing deformities. Try not to apply socks that are too tight..
- Trim nails, corns and bunions cautiously; we recommend having this done in our office as nails not cut properly can become ingrown, prompting infection, ESPECIALLY in our diabetic patients. Corns and calluses that are cut too short can create wounds and can also lead to infections.
- Shield feet from outrageous temperatures
- Get ordinary assessments on the feet: Regular assessments by a specialist are critical to preventing infections, amputations, and serious diseases.
- Control glucose: Uncontrolled blood sugars increase the danger of podiatric complications from diabetes.
- Abstain from smoking: Smoking decreases oxygen within the bloodstream of the tissues, which can aggravate foot in individuals with diabetes.
Treatment of Diabetic Foot:
A scope of nonsurgical and surgical choices are available.
Nonsurgical treatment
A specialist will initially treat diabetic foot issues without utilizing a surgical procedure. A few strategies include:
- keeping wounds clean and dressed
- wearing immobilization devices, for example, a boot or total contact cast
Surgical treatment
At the point when nonsurgical treatment doesn’t effectively treat diabetic foot issues, the specialist can utilize the most up to date Limb Salvage procedures at Port St Lucie. These treatment options are on a case by case basis and we suggest seeking the consultation of a foot and ankle specialist to guide you appropriately.
What is limb salvage
The answer is in the name. Through the use of offloading techniques, medical equipment, surgical reconstruction and multidisciplinary medical approaches, our physicians are highly trained to do anything and everything to preserve and save the limb, whether that be the foot, ankle or leg.This encompasses patients with diabetic foot ulcers, leg wounds, bone infections, foot infections, abscess formation in the foot, charcot neuroarthropathy and so much more. If you are diabetic and find yourself suffering from ANY symptoms or complications within your foot and ankle, schedule an appointment today with your Saint Lucie County Diabetic Limb Salvage specialist at Harlis Family Foot and Ankle.

Hallux Rigidus
Hallux rigidus is a common arthritic condition of the big toe joint. It can cause hallux toe pain, pain when walking and when exercising. There are various hallux rigidus stages, but generally, the condition is classified based upon severity and destruction at the joint.
What causes Hallux Rigidus?
Hallux rigidus is so common because there are many different causes. Actually, many of these are the same as hallux valgus causes, or causes associated with developing a bunion. Some of these include a hypermobile first ray (which is also associated with both mild and serious hallux valgus), metatarsal elevatus, where the metatarsal bone is elevated with respect to the ground, arthritis, trauma, neuromuscular disease, and the list goes on.
What are some Hallux Rigidus Symptoms?
Based upon the hallux rigidus stage you are in, there may or may not be symptoms. For instance, in the final stage of hallux rigidus, there usually is no associated pain because at that point, the joint between your hallux or great toe, and the first metatarsal has fused. However, in lesser stages of Hallux Rigidus, a patient tends to have decreased range of motion in the big toe joint, gradual pain at the big toe joint with walking, and a boney prominence at the top of the big toe joint. Luckily, there are a number of hallux rigidus treatments employed today, and the physicians at Harlis Family Foot and Ankle in Port Saint Lucie are your local experts!
Hallux Rigidus Treatments
There are many treatment options for hallux rigidus that include both surgical and non-surgical methods. Unfortunately, there are not many hallux rigidus exercises that are commonly employed, but generally, putting your big toe through range of motion if not painful can be helpful. The physicians and surgeons at Harlis Family Foot and Ankle in Port Saint Lucie are also able to fit patients with different shoes that can help with walking, and administer steroid injections if the area is painful.
Sometimes patients fail conservative treatment measures and are forced to consider surgical options. Hallux rigidus surgery can be performed in different ways. For instance, the surgeon can decide to perform a bunionectomy, clean up the joint by removing bone spurs, fusing the joint, and even doing a joint replacement. The possibilities are endless, and The physicians and surgeons at Harlis Family Foot and Ankle in Port Saint Lucie have received comprehensive and extensive training in all of these modalities.
If you find you are suffering from this potentially painful issue, please book an appointment with one of our surgeons today!

Lisfranc Injuries
Have you recently or in the past experienced a foot injury that caused severe pain to your arch and the middle of your foot? If so, you may have sustained a Lisfranc injury. A Lisfranc injury may constitute a broken bone, or fracture dislocation in the middle of your foot, or may just be an injury to a vital ligament. Whatever the reason, the physicians and surgeons at Harlis Foot and Ankle are specifically trained to handle these types of ailments.
What is the Lisfranc Complex?
The Lisfranc complex is a joint in the middle of your foot where your metatarsal bones, i.e., the long bones in the middle of your foot, link to the remaining foot.
It is an extremely complex area of the foot because it is where all the tendons, ligaments, and bones join and work in conjunction to maintain your arch. So, as a part of your joint system, all elements interact at this point. The importance in your normal foot architecture cannot be understated. You can consider it the main intersection in your city’s busiest highway.
Unfortunately, any part of the Lisfranc Complex can be compromised, and as previously stated can be a fracture (sometimes this is referred to as a midfoot fracture) or lisfranc sprain. A Lisfranc fracture dislocation or sprain usually occurs from a traumatic injury. Athletes sometimes damage this joint while playing sports, and injuries can also occur from tripping or stumbling. High velocity or more major events like falling from a ladder and car accidents cause Lisfranc fracture-dislocation. If you sustain a fracture, you might damage one bone, but you can still damage the surrounding soft tissue. symptoms include foot and ankle pain, and swelling.
Is there any treatment for the Lisfranc injury?
Yes, there are two types of treatment options:
- Non-surgical treatment (Conservative care management)
- Surgical treatment
If you believe you may have sustained a Lisfranc injury, immediately present to your nearest hospital or urgent care facility. If you have a podiatrist that you see, you can call them as well. At Harlis Family Foot and Ankle, we accept same day appointments and never turn away emergencies. We also have x-ray capabilities to quickly evaluate the severity of any given injury.
Conservative care management or Non-Surgical Treatment
If symptoms are mild, and a fracture is not identified. You doctor may advise the following:
- Do cold compresses and apply compression to the painful area
- Elevate the foot as much possible
- Resting the injured foot
- Immobilization in a cast or boot
- Non-weightbearing
Surgical Options:
Surgical intervention is indicated if your ligament and bones have shifted from normal anatomical alignment or show evidence of severe damage. As before stated, this will usually occur after high velocity accidents or major trauma. The surgeon uses orthopedic hardware such as plates and screws to reduce and fixate the injury, and allow the soft tissue and bones to heal
Recovery Period:
After surgery, you will need to be immobilized for at least 6-8 weeks and have serial x-rays performed to ensure adequate healing. With a sprain, the recovery period is similar depending on your symptoms. As with any injury, clinical presentation and recovery can vary depending on the patient, which is why it is important to closely follow up with your doctor, and strictly adhere to their recommendations.
If you feel you have suffered a Lisfranc injury and are in the Port St. Lucie area, don’t hesitate to contact our physicians and surgeons at Harlis Family Foot and Ankle.

Minimally Invasive Surgery
The goals of any Minimally Invasive Surgery (MIS) are generally to allow a less noticeable scar and promote faster recovery times. When it comes to MIS of the Foot and Ankle, these principles still hold true. Our surgeons are minimally invasive procedure specialists at Port St. Lucie. Our commitment is to use the smallest incision possible to perform reduction and correction of deformities.
These minimally invasive procedures provide an excellent option when considering food and ankle surgery. Some benefits of minimally invasive surgery are:
- Decreased pain following surgery
- Decreased manipulation of soft tissues
- Decrease in chances of infection
- Decrease in surgical site dehiscence
- Faster recovery times vs traditional open surgeries
What is minimally invasive surgery?
Our surgeons utilize percutaneous, micro incisions to correct a number of different foot and ankle deformities including, but not limited to: bunions, hammertoes, hallux rigidus (arthritis of the great toe), flat foot, heel spurs, and many other foot conditions. Through the use of MIS techniques, far less damage occurs to our patient’s foot, due to the decrease in tissue manipulation.
Whenever possible, we try to implement MIS techniques, however, there are instances that use of traditional, and larger incisions must be implemented. But, fear not. Our surgeons have been thoroughly trained to be able to perform surgeries using both MIS and traditional techniques, and even when we pursue traditional open techniques we always try to perform through the smallest incision possible for less invasive surgery. For more information, please consult with a podiatrist.

Osteochondral Lesion of Talus
Do you have pain and swelling in the ankle and hear popping and/or clicking sounds? You could have an Osteochondral lesion of the Talus. Visiting your local foot and ankle specialist will give you a better indication of what exactly is happening, after they run tests like x-rays. Sometimes more advanced imaging may be required such as a CT or a MRI. From there they will determine if you do truly have an Osteochondral lesion of the ankle.
But what is it??
An OCD lesion of the ankle is a fracture of the cartilage. Normally cartilage provides for smooth movement in joints, but when fractured it can cause pain and popping noises as that cartilage moves around in the ankle.
How does it occur?
It usually happens from a traumatic injury to the ankle. This situation may arise if your ankle is unstable or misaligned. Let’s deep-dive to understand talus and talus injury:
What are Talus and Talar dome injuries?
The talus is a bone of your foot, together with a tibia, and fibula hat makes up your ankle joint. Talus is a dome-shaped area, and it is totally covered by the cartilages that allows for smooth joint movement. In a talus injury, this cartilage can be torn or fractured whenever your ankle joint gets damaged or hurt and causes the talus’s osteochondral lesion.
In some cases, the piece of talus cartilage might break off but remain there. Another name for this ailment is a talar dome lesion. This condition may cause severe ankle pain and swelling, and if not treated on time, it can permanently damage the joint.
What are the symptoms of OCD lesion ankle?
In an osteochondral lesion, the symptoms develop gradually and slowly. Following are its symptoms
- Swelling
- Ankle giving out
- catching or clicking sensation when walking
- chronic pain
Treatments of the OCD lesion ankle
So there are two types of treatment that you can follow or your doctor suggests:
- Conservative care management
- Surgical management
Conservative Care Managements
The conservative or non-surgical treatment is effective when the doctor diagnoses the Talus injury early. These treatments include but are not limited to:
- wearing a brace or cast to minimize stress and promote the healing of the ankle
- Physical therapy
- Steroid injections
- also, Nonsteroidal anti-inflammatory drugs
Surgical management
If the primary treatment is ineffective and the condition worsens, the doctor may recommend surgery. It is a must to restore the movement and alleviate the pain.
- Ankle arthroscopy to clean and clear ankle joint of damaged cartilage. Arthroscopy is not an invasive procedure that needs limited incisions and causes less pain and speedy recovery.
- Bone/Cartialge grafting
The Timeline for recovery: OCD lesion ankle
- The recovery time after the Talus lesion is from 6 months to one year. The motion exercises to light CVS exercises can straighten the joint.
- For 2 or 3 days after surgery, most people are advised to stay off their feet and take rest. You might be capable of moving around after about 3 days.
For more information, please consult with our podiatrist at Harlis Family Foot and Ankle.
