
- Achilles Tendonitis
- Ankle Instability
- Ankle Pain
- Ankle Sprains
- Athlete’s Foot
- Bunions
- Corns
- Calluses
- Diabetic Foot Care
- Flat Feet
- Geriatric Foot Care
- Gout
- Hammertoes
- Heel Spurs/Plantar Fasciitis
- Ingrown Toenails
- Neuromas
- Pediatric Foot Conditions
- Peripheral Neuropathy
- Toenail Fungus
- Warts
- Foot Fractures
- Foot and Ankle Surgery
- Foot Pain

Achilles Tendonitis
Achilles tendinitis is caused by overuse of the band of tissues that connects the lower region of your calf muscle to your heel bone, also known as your Achilles tendon. Those at a higher risk for Achilles tendinitis are runners engaging in intense training or middle-aged people who participate in sports on occasion.

Ankle Instability
Chronic ankle instability is usually caused by repeated ankle sprains and is described as the gradual giving way of the outside of the ankle. Some symptoms of ankle instability include constant inflammation or swelling, tenderness, and instability in the ankle. After a sprained ankle, the ligaments become stretched and torn. Proper rehabilitation is required to strengthen the muscles around the ankle and rehabilitate the tissues within the ankle that affect your balance. In addition, physical therapy, medications, and bracing can help treat chronic ankle instability. Failure to do so may result in repeated ankle sprains, or possibly surgery.

Ankle Pain
The foot and ankle are highly specialized structures that absorb the weight of the body and enable us to move. Experts estimate that the force and pressure on your feet when walking can be up to two times your body weight. This pressure can increase with more vigorous movements such as running and jumping. With so much pressure on your feet and ankles, they undergo a lot of wear and tear throughout your life and are highly susceptible to injury and trauma.
The foot and ankle are a complex system of bones, ligaments, muscles, and joints that provide the structure and stability we need to move freely. If any of these components become compromised or weakened due to injury, overuse, degenerative conditions, or sprains, it can significantly impact your foot’s ability to move and function properly.

Ankle Sprains
A sprained ankle occurs when you twist your ankle in an abnormal way causing the ligaments holding your ankle bones together to stretch or tear. Most sprained ankles involve injuries to the ligaments on the outer side of the ankle. Treatment for a sprained ankle depends on the severity of the injury. Although you may just need proper rest and pain medications to heal, it is important to have the sprain looked at by a professional to determine the severity and proper treatment.

Athlete’s Foot
Athlete’s foot (tinea pedis) is a specific type of fungal infection that typically begins between the toes. A common cause of athlete’s foot is sweaty feet that are confined to tight shoes for a long period of time. Signs and symptoms of athlete’s foot include a scaly rash that usually causes itching, stinging and burning. Athlete’s foot is contagious and should be carefully monitored and treated. Athlete’s foot can easily be treated with antifungal medications, but the infection is likely to recur. Prescription medications also are available.

Bunions
A bunion is a bony bump that forms on the joint at the base of your big toe. They can develop from an inherited structural defect, excess stress on your foot, or can result from an existing medical condition.
For the most part, bunions require no medical treatment. However, if you are experiencing one or more of the following, a podiatrist can help alleviate your symptoms.

Corns
Corns tend to be smaller than calluses and are the hard center is surrounded by irritated skin. While corns can be found on the bottom of the foot where pressure is usually applied, it is more common that you find corns on the tops and sides of your toes and even between your toes. When pressure is applied, corns can cause significant pain and discomfort.
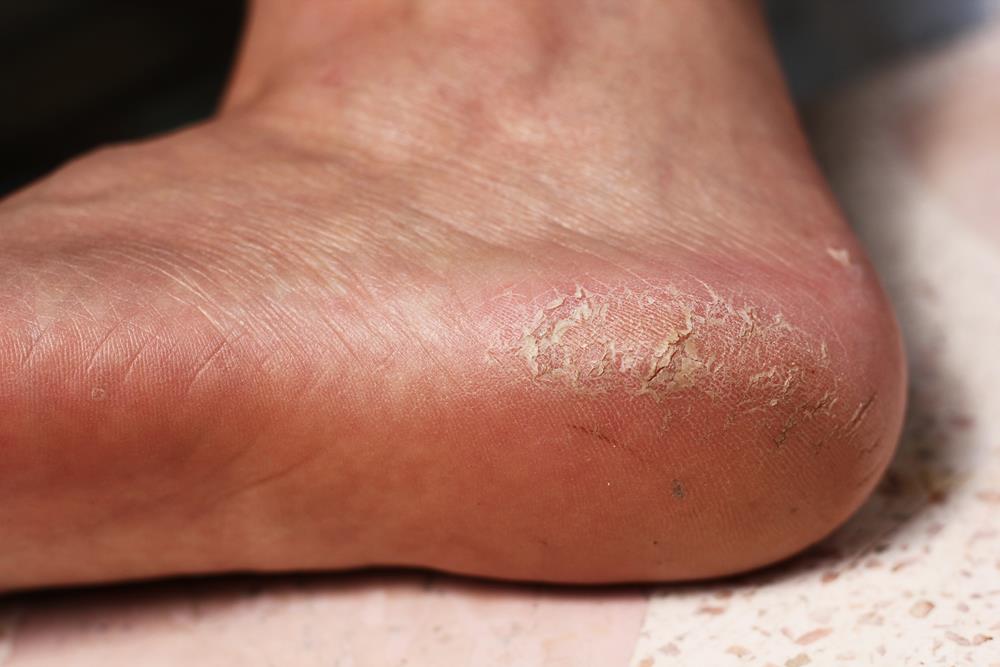
Calluses
Calluses, on the other hand, don’t usually cause pain. They usually develop on the soles of your feet, especially under the heels or balls, on your palms, or on your knees. Calluses vary in size and shape and are often larger than corns.

Diabetic Foot Care
Daily preventative care can help you decrease your risk of developing these other serious conditions like ulcers and infections. Inspecting your feet at the end of the day to look for any abnormalities, maintaining proper hygiene, keeping your feet warm in cold weather, encouraging blood flow in the feet, and maintaining an overall healthy lifestyle can discourage other conditions from developing.

Flat Feet
Painful pes planus or “flat feet pain” is an extremely common problem causing over 3 million medical visits in the US every year. Flat feet problems are treated in our practice regularly, and our doctors at Harlis Family Foot and Ankle are especially trained to do so.
What are flat feet and what causes flat feet?
All babies are born without arches, which usually develop by approximately age six. When arches fail to develop during childhood, this is a condition known as flat feet, or pes planus. Flat feet are characterized by feet that have no arch and when the middle of the foot is flush with the ground.
Causes of Flat Feet
There are many possible causes of flat feet, including:
• Genetics
• Obesity
• Pregrancy
• Old age
• Rheumatoid arthritis
• Injuries such as a broken bone or Achille’s tendon injury.
The likelihood of having flat feet increases in those with diabetes or certain muscular or neurological diseases such as muscular dystrophy, spina bifida, or cerebral palsy.
Different Types of Flat Feet
Not all flat feet are the same. In adults, flat feet are categorized as either rigid or flexible.
Rigid flat feet. Individuals with this type of flat feet will have no arch at any time: when putting weight on the feet or when sitting, when there is no weight on the feet.
Flexible flat feet. Arches in individuals with flexible flat feet will be visible when sitting or while on tiptoes. However, the arches will collapse once standing and when weight is put on the feet.
Adult-acquired (fallen arch). This is a sudden drop or collapse of the arch which may only affect one foot. It can be caused by inflammation or a tear in a leg tendon that supports the arch.
Vertical talus. This is a congenital disability where the ankle’s talus bone is improperly positioned, causing the bottom of the foot to look like a rocking chair’s bottom.
Symptoms of Flat Feet
Flat feet are often asymptomatic, however many people can experience one or more of the following symptoms:
• Arch pain
• Ankle pain
• Heel pain
• Stiffness
• Changes in gait
• Muscle pain or fatigue in the feet or legs
• Toe drift
• Balance issues or difficulty standing
Diagnosing and Treating Flat Feet
To make a diagnosis, a podiatrist will observe your feet as you sit, stand, and walk, and will assess your symptoms. In some cases, they will want to evaluate bone structure by looking at an X-ray.
Depending on the type of symptoms and severity of the condition, a podiatrist may treat flat feet with custom orthotics/shoes, foot braces, nonsteroidal anti-inflammatory drugs (NSAIDs), or ice and rest. They may suggest physical therapy to improve flexibility and strengthen muscles and tendons.
If flat feet are interrupting your daily activities or causing you any discomfort, have your condition evaluated and treated by a podiatrist.

Geriatric Foot Care
Taking care of ourselves as we age should be a priority. We want to live as long as we can, and have the best quality of life possible. While other aspects of our physical health may take priority, it is equally important to be proactive about our foot and ankle health, as mobility is a key to independent living as we get older.
Foot and ankle conditions among geriatric patients are often due to complications of systemic diseases such as arthritis, diabetes, and circulatory issues. The feet are often the first place where symptoms of these diseases present themselves. So, it is important to be vigilant in detecting early signs of these diseases and seek treatment as soon as possible.
Diabetes and Geriatric Feet
Many older adults have diabetes which can lead to foot problems. Nerve damage associated with diabetes can make it difficult for older adults to detect tiny cuts, abrasions, or hot spots on the feet. Poor circulation also brought on by diabetes can compound this problem by making it difficult for the body to heal even the most minor skin disturbance. That is why it is important for aging adults to inspect their feet and toes every day for any type of cut, bruise, red spot, corn, callus, etc., and see a podiatrist right away if anything unusual is detected. Regular visits to the podiatrist are essential for diabetics to facilitate optimal foot health and early prevention when necessary.
Arthritis and Geriatric Feet
Early detection and treatment can help the elderly patient and their podiatrist manage arthritic symptoms more effectively. It can also help maintain joint functionality and decrease the risk of any potential disability. Any pain, swelling, or stiffness in the feet or ankles should prompt a visit to the podiatrist for diagnosis as soon as possible.
Other Geriatric Foot Conditions
Other common foot and ankle disorders among the elderly include:
• Heel pain
• Ingrown toenails
• Fungal toenails
• Dry skin and cracked heels
• Dorns and calluses
• Bunions
• Hammertoes
• Gait anomalies
Geriatric Foot Care Tips
The following foot care tips can often prevent these issues from developing, and will help older adults maintain optimal foot and ankle health:
• Check feet regularly to monitor foot health and report cuts, sores, or anything unusual to your podiatrist.
• Keep the blood flowing by walking daily, and doing gentle stretching exercises for the feet and toes.
• Try to avoid sitting for long periods of time, and elevate the feet as much as possible.
• Be sure to wear comfortable shoes that fit well and offer ample room in the toe box along with support in the heel and arch.
• Wear moisture-wicking socks that fit comfortably and do not put pressure on any part of the feet or ankles.
• Wash and dry feet thoroughly every day to keep infections at bay, and moisturize them to avoid dry or callused skin.
• Never walk barefoot, even around the house.
• Keep toenails trimmed straight across but not too short, which may lead to an ingrown toenail. A podiatrist can trim nails for those who cannot do it themselves.
• Do not smoke. Smoking reduces blood supply and may exacerbate swelling and circulatory problems.
• Maintain a healthy body weight by eating a well-balanced diet and staying active.
• Foot pain and decreased mobility is not normal and should not be ignored. Make an appointment with a podiatrist for an examination as soon as possible.
A podiatrist is an essential part of the older adult’s team of healthcare providers. Make an appointment today to learn more about how to keep feet and ankles healthy in order to maintain an active, independent lifestyle.

Gout
Often we associate arthritis with older patients who have lived an active lifestyle. Gout, on the other hand, can affect anyone. Gout is a common form of arthritis that is known for its sudden attacks of pain and joint tenderness. Joints that are affected by gout are often hot to the touch, swollen, and very tender. While symptoms are not chronic, it is essential to take preventative measures to manage gout as its side effects can be debilitating and intolerable.
- Stay hydrated. By drinking plenty of fluids and limiting sugary drinks, you can help prevent future gout attacks.
- Maintain a healthy weight as directed by your healthcare provider.
- Limit alcohol consumption. Some types of alcohol are more likely to increase the likelihood of a gout attack.
- Consider adding low-fat dairy products to your diet. These foods are proven to help protect against gout and are excellent sources of protein.

Hammertoes
Hammertoe is a deformity where one or both joints of the second, third, fourth or fifth toes begin to bend outside of their normal alignment. Pressure can begin to weigh heavy on the toes as you wear shoes which is where pain and other symptoms develop.
Hammertoes typically begin with small symptoms and deformities and continue to worsen with time. In its beginning stages, hammertoes are often impressionable which means they can be controlled using minimal treatment. It is important to know the signs of hammertoes to get them evaluated early. If left untreated, hammertoes can become more firm and difficult to manipulate, requiring surgery.
Heel Spurs/Plantar Fasciitis
Heel Spurs are boney protrusions that develop on the bottom edge of the heel bone when it sustains repeated stress and the body sends calcium to the area in response. This extra calcium builds up over time to form sharp outgrowths on the bone that can sometimes reach 1/2” in length.
What Causes Heel Spurs?
Heel spurs are caused by damage or bruising to the heel bone. They are commonly caused by plantar fasciitis, and both conditions can occur at the same time.
Plantar fasciitis is a condition where the plantar fascia tissue that runs along the bottom of the foot, connecting the heels with the toes, becomes overly stretched, worn down, or torn. This causes repeated irritation on the heel bone where the tissue inserts and triggers the body’s attempt to heal by releasing calcium to the site. The heel spur begins to develop over months or even years.
Heel Spur Symptoms
Heel spurs are often asymptomatic and are only discovered on an X-ray. If they are symptomatic, they can cause intermittent or chronic pain, inflammation, and tenderness at the bottom of the heel.
Heel Spur Risk Factors
The following are factors and situations that may increase the risk of plantar fasciitis and heel spurs developing:
• Obesity or sudden weight gain, which puts undue stress on the plantar fascia and heel
• Having to stand at work all day
• Ill-fitting, unsupportive footwear that puts strain on the arch and alters one’s gait
• Repetitive movements or high-impact physical activity (like running on hard surfaces) that overly stretches or wears down the plantar fascia tissue
• Age, which can make the plantar fascia less flexible and thin down the heel’s fat pad
• Diabetes, which can cause hyperglycemia, weight gain, and weaken or thicken the plantar fascia
• High Arches or Flat Feet
Treatment of Heel Spurs
A podiatrist may use one or more of the following measures to help treat heel spurs:
Resting and Icing: If heel spurs are symptomatic, a podiatrist may use icing to reduce pain and inflammation. They may also recommend refraining from physical activities that attributed to the formation of the heel spurs and resting the feet throughout the day.
Proper Footwear & Orthotics: Podiatrists can make professional recommendations on footwear to help relieve symptoms. They may also prescribe custom-designed and fitted orthotics which can relieve pressure from the heel spur and support the arch.
Physical Therapy: Certain exercises, physical therapy, lower leg strengthening, and massage can also help reduce the pain and inflammation of heel spurs, while increasing mobility and flexibility.
Taping & Night Splints: Techniques such as arch support taping or night splints can often help heal the plantar fascia and reduce symptoms of heel pain and plantar fasciitis.
Medications: A podiatrist may recommend over-the-counter oral medications and/or corticosteroid injections to reduce pain and inflammation.
Surgery: If conservative measures fail to provide relief after approximately one year, your podiatrist may recommend surgery to remove the heel spur and treat the plantar fasciitis that may have contributed to its formation.
If you believe you may have a heel spur, make an appointment with a podiatrist to have your condition properly diagnosed and treated.
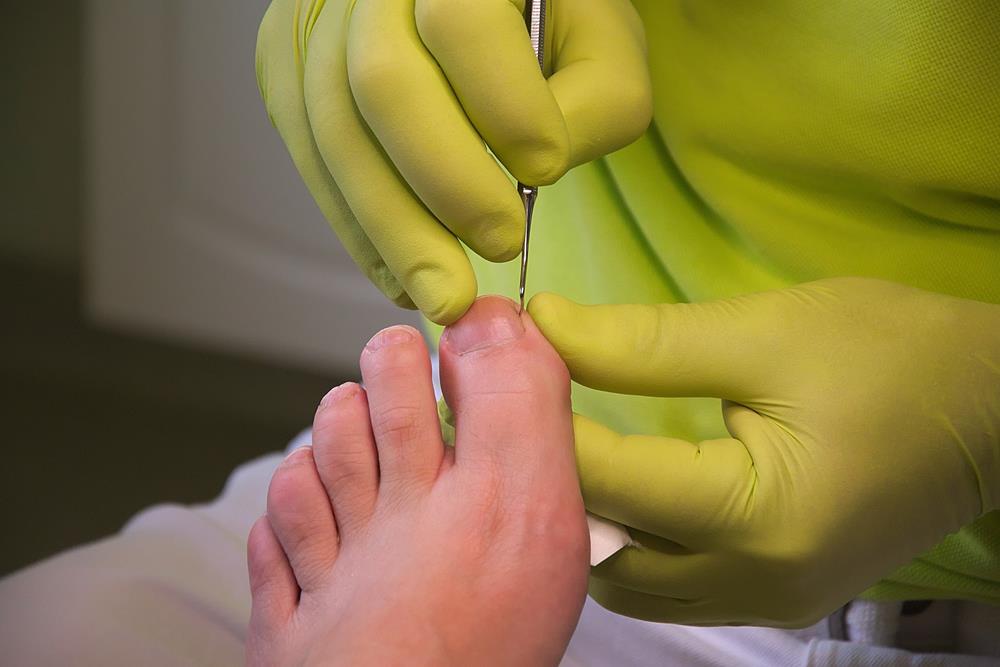
Ingrown Toenails
We have all made the painful mistake of trimming our nails too short at some point in our lives. Sometimes, this can really affect our foot health by causing ingrown toenails.
This happens when the nail grows downward into the skin instead of straight out, usually causing an infection. Ingrown toenails are most common on the sides of the big toe. It can also be caused by shoe pressure, injury, fungal infections, poor foot structure, etc.
Warm water soaks several times a day, properly fitted shoes and socks, and trimming nails in a straight line (rather than rounded) are ways to treat and prevent painful ingrown toenails. If there is an infection, antibiotics may be prescribed.

Neuromas
Morton’s Neuroma, also known as inter-metatarsal neuroma, is a thickening of tissue around the nerve that runs between the third and fourth toes.
The thickening of nerve tissue is the body’s response to the nerve being compressed or irritated. This irritation is often caused by wearing high heeled shoes that force toes into the toe box or other pointy footwear that squeeze the toes together.
Flat feet, bunions, and hammertoes can also contribute to the formation of Morton’s neuroma as well as injuries and participating in physical activities which repeatedly stress the ball of the foot, like court sports or running.
Symptoms of Morton’s Neuroma
Morton’s neuroma is a progressive condition. At first, symptoms may come and go, only occurring during activity or when wearing certain shoes. As time goes on and the neuroma gets bigger, the symptoms will worsen.
Because of the location of the nerve that is affected in Morton’s Neuroma, symptoms are typically felt in the ball of the foot:
• Pain
• Tingling
• Numbness
• Burning
• The sensation that a sock is bunched up in the front of the shoe
• The feeling of having a pebble stuck in your shoe
Diagnosing and Treating Morton’s Neuroma
To make a diagnosis of Morton’s neuroma, your podiatrist will need to perform a physical examination, run various tests, and may need to evaluate diagnostic imaging.
There are both conservative and surgical treatments for Morton’s neuroma. An early detection of this condition increases the chance that it can be treated conservatively.
Conservative (non-surgical) treatments include:
• Icing the affected area
• Wearing custom orthotics and padding to lessen compression and pressure on the nerve
• Taking nonsteroidal anti-inflammatory medications to reduce inflammation and pain
• Making modifications to footwear to allow for more room in the toe box
• Getting cortisone or other types of injections to reduce inflammation and pain
Surgical treatment. If the condition does not respond properly to more conservative treatments, your podiatrist may recommend surgery to remove the nerve and release ligaments that are tight in the surround area.
Morton’s neuroma is not only uncomfortable, but if left untreated, may lead to permanent damage. Call a podiatrist as soon as possible if you have any of the symptoms listed here.

Pediatric Foot Conditions
Pediatric foot deformities is a term that incorporates a scope of conditions that might influence the bones, ligaments, and muscles of the foot in young children. Usually when parents bring in their children complaining of a delay in their child’s ability to walk they use phrases such as legs that won’t walk, bowed legs of baby, flat foot baby, or walking with feet outward. And although these can be reasons for late walking in babies, there usually is a underlying medical diagnosis. But fear not at our medical facility at Port Saint Lucie, Florida, we can evaluate and diagnose the appropriate condition that might be affecting your young one.
Treatment of foot deformations in adolescents can vary greatly from that required in adults. Luckily, pediatric orthopedists who have expertise in this field can bring usable strategies explicitly created to address the particular necessities of kids, which incorporate exceptional thoughtfulness. Below are some of the foot and ankle deformities seen in children.
Cavus Foot:
Cavus foot is a condition where the youngster has an exorbitantly high arch. By and large, the impact point of the foot is turned internal (this is known as cavo varus foot deformation). Patients experience pain and calluses on points where their feet contact the ground.
Tarsal Coalition
Kids with tarsal coalition have an unusual fusion between the bones in the midfoot or hindfoot. It is generally analyzed in late youth or early adulthood when the alliance starts to restrict foot development, causing pain and ‘locking up of the foot’. Manifestations might be especially recognizable when walking on a lopsided surface, like sand or rock, an activity that requires steady change of the foot. Routine lower leg injuries may likewise alert the presence of a coalition.
Clubfoot :
Clubfoot is a condition where the two feet are turned internal and are pointing down. Quickly evident upon childbirth, clubfoot is known to happen during intrauterine life, at somewhere in the range of 9 and 14 weeks incubation. Indeed, as a rule, the distinction is recognized on routine ultrasound. It is a lot simpler for parents to adapt and arrange for when they know ahead of time what they need to do.
Happening in around one of every 1000 births, clubfoot is routinely seen more in young men than in young ladies. Furthermore, albeit family ancestry might have an impact, numerous newborn children with clubfoot have no known relatives with the condition.
In most cases, clubfoot can be effectively treated without a medical procedure, utilizing the Ponseti strategy, which uses delicate control and correction of the feet on a weekly basis. Treatment starts not long after birth when the infant’s feet are generally responsive. Following this first period of treatment, a cast is utilized over a period of time. When applied accurately, the Ponseti procedure yields incredible outcomes.
We have the expert doctors up for your help. If you have questions regarding your child’s foot and ankle deformity, come see a podiatrist at Harlis Family Foot and Ankle in Port Saint Lucie, Florida.
Peripheral Neuropathy
As a result of damaged peripheral nerves, peripheral neuropathy can occur causing symptoms like weakness, numbness, burning, and tingling in the hands and feet as well as other parts of the body. Traumatic injuries, diabetes, and even some exposure to toxins can cause peripheral nerve damage.
Once damage to nerves occurs, the symptoms of peripheral neuropathy are gradual and worsen with time. It is important to maintain a healthy lifestyle to aid in the prevention of damage to those specific nerves.
request an appointment
Toenail Fungus
Fungal infections in the toe or fingernails can appear as thickened, discolored, or disfigured. While it may seem like the condition is just an aesthetic concern, fungal infections can lead to worsened symptoms and pain. Diabetes, a weakened immune system, and the normal aging process are all causes associated with fungal infections. It is more likely for senior citizens and adults to develop a fungal infection as opposed to children.

Warts
Plantar warts are caused by the HPV virus and cause tiny cuts and breaks on the bottom of your feet.
While most plantar warts are not a major health concern, it is advised you see a doctor to have the warts examined and removed. Some symptoms include small, rough lesions on the base of the foot, calluses in one spot, and tenderness when walking or standing for long periods of time.

Foot Fractures
There are a series of different injuries that can occur in the foot and ankle ranging from injuries relating to foot ankle tendons, foot ligaments injuries, and broken ankle and foot bones. As anyone who has experienced foot and ankle injuries can tell you, ankle and foot pain can be debilitating as there’s pain with literally every step. Depending on the injury our doctors will likely recommend some form of immobilization through the use of a boot but it is extremely important to not attempt to make an ankle injury diagnosis and buy a boot. If you find yourself in this category (and you shouldn’t be!!) under no circumstances should your walking boot be causing ankle pain. Even if you were seen by a specialist and you are having pain while in a boot, you should contact them immediately. Below you will find more information on a couple of foot and ankle trauma diagnosis.
Ankle Fracture Treatment:
Ankle fracture treatment depends on the arrangement of the bones and the stability of the ankle joint. In the event of an unstable ankle fracture, surgery is required. The objective is to have anatomic reduction of the fracture with great alignment. A misalignment of just two millimeters in the lower leg joint can lead to increased risks of post traumatic arthritis. Certain fractures can be dealt with non surgically with a brace, short leg cast, or other off loading device. Some patients might have the option to walk immediately while wearing a boot, while others might need to restrict weight bearing.
For more serious breaks where surgery is required, patients ordinarily do not bear weight for a month and a half until the bone mends. For the primary two or three weeks, patients are in a posterior splint and are elevating the appendage 90% of the day. Following 10 to 14 days, the stitches are taken out and patients are ordinarily positioned into a removable boot. This permits patients to begin moving the lower leg (active range of motion) and to shower. Throughout this process, X-ray imaging are taken to look at boney healing.
Assuming the bone is healed well; patients are then permitted to begin weight bearing and to start ankle fracture physical therapy (sometimes physical therapy is started prior to weight bearing). This is pivotal in helping to stabilize ankle fractures. Patients will by and large have a minimum of a month and a half of treatment or more.
Regardless of whether surgery is required or not, it generally takes around a month and a half for bones to completely heal. However, it might take more time for tendons or soft tissues to completely recover.
There is always a question as to what to do for a fractured ankle and how long it takes for an ankle fracture to heal. Our specialists at Harlis Family Foot and Ankle can assist you in ankle injury treatment at Port St Lucie and will guide you on how to heal a fractured ankle.
Jones Fracture
A Jones fracture can be a debilitating diagnosis. It is commonly seen amongst athletes and in high energy, high torsion injuries. Usually patient have symptoms consistent with pain to the outside of their foot, difficulty walking, along with swelling. It is also fairly common to see jones fracture bruising, at the outside of the foot. There are a couple of different ways to approach jones fracture recovery/treatment of these injuries and these are all patient specific. That is what we specialize in at Harlis Family Foot and Ankle; patient specific treatment plans. If you find yourself with this possible diagnosis dont worry as our physicians offer the best jones fracture treatment at Port St Lucie.
Some of the most common questions/comments we have with patients that have a Jones fracture are: what are the best shoes after jones fracture, how to heal a jones fracture faster, how to increase blood flow to jones fracture, long term effects of jones fracture and how long is jones fracture recovery. Unfortunately there is no ‘one size fits all’ answer for every patient. But thankfully, these are all questions that our highly trained doctors can answer. If you need treatment for jones fracture at Port St Lucie, visit us at Harlis Family Foot and Ankle.
Calcaneal fracture
A calcaneal fracture is a heel bone fracture/ fracture of the heel bone. These are routinely seen when patients fall from heights. Most commonly when falling from ladders or from roofs, so it is no surprise that the Christmas season brings a lot of these patients into the office. Some patients are unfortunate to have bilateral calcaneal fractures Common symptoms are inability to walk, pain in the back of the foot, swelling, and calcaneus fracture bruising. Unfortunately these are not considered minor fractures and life after a calcaneus fracture, if not treated properly (and even when treated properly) can be debilitating. However fear not, our highly trained physicians can work with you to develop a plan to help ensure your success.
When patients fall from heights and experience these symptoms, they are not considered a minor heel fracture. The only time a calcaneal fracture is considered ‘minor’, is if it is a stress fracture which occurs from repeated activities that overstress the bone inducing the fracture. But sometimes those can progressively worsen and become an issue. If you are seeking calcaneus fracture treatment at Port St Lucie, or heel fracture treatment at Port St Lucie, come and visit a podiatrist at Harlis Family Foot and Ankle.

Foot and Ankle Surgery
If your podiatrist suggests foot or ankle surgery, it is most likely because more conservative approaches have not provided optimal results. Or, your condition may be an acute injury that requires immediate surgical intervention.
Examples of Foot and Ankle Surgery
Foot and ankle surgery can treat a variety of conditions and injuries. Surgery may be needed to align broken bones, fix a deformity, reconstruct or fuse a joint that has been ravaged by arthritis, repair torn tendons or ligaments, or remove damaged or diseased tissue.
• Fractures: Surgery is often necessary when a foot or ankle fracture has caused the bone to be displaced or misaligned. Surgical intervention is then needed to restore functionality and reduce the risk of deformity.
• Bunion and hammertoe correction: Bunions and hammertoes are foot abnormalities that sometimes need surgery to properly reduce pain and correct the deformity permanently. There are various types of procedures (some are minimally invasive) to straighten and stabilize tendons, bones, and joints in both of these conditions.
• Ankle surgery for arthritis: When arthritis has severely damaged the ankle and pain, inflammation, and loss of mobility affects the patient’s quality of life, ankle surgery may be necessary. Ankle fusion fuses a leg and foot bone in one piece at the ankle. Ankle replacement uses metal and plastic prosthetics to replace damaged cartilage and bone in the ankle. Minimally invasive procedures are sometimes an option in these types of procedures.
• Achilles tendon repair: When tendons such as the posterior tibialis tendon or the Achilles tendon degenerate over time or suffer an acute tear or rupture, surgery may be required to properly fix the tendon, relieve pain and inflammation, and restore functionality. These types of procedures can sometimes be minimally invasive.
• Ankle stabilization: Repeated ankle sprains or an improperly healed sprain can sometimes cause chronic ankle weakness. A lateral ankle ligament reconstruction may be suggested to tighten up the ligaments on the outside of the ankle to stabilize it, eliminate chronic pain and prevent future sprains from occurring.
• Wound debridement: This is a procedure that removes dead tissue from a diabetic foot wound or ulcer to help it heal and prevent an infection from occurring or worsening. There are additional surgical interventions that podiatric surgeons may perform in the treatment of diabetic ulcers such as skin grafting and vascular surgery.
To learn more about what foot or ankle surgery might be right for your condition, consult with your podiatrist.

Foot Pain
The foot is composed of 26 bones, 33 joints, along with muscles, ligaments, and tendons. The foot’s complexity, and its role in bearing the weight of the body, can lead to various painful conditions and injuries.
Foot pain, and associated symptoms such as inflammation and limited mobility, may be caused by:
• Traumatic injuries
• Overuse injuries (develops over time)
• Genetic or acquired deformities
• Muscle imbalances
• Poor training form
• Systemic diseases (i.e., diabetes or arthritis, ill-fitting shoes, obesity, or infections)
Where Can Foot Pain Occur?
Foot pain can be generally categorized by where it occurs: the toes, the arch, the heel, or the ball of the foot.
Toe pain can be the result of fractures, ingrown or fungal toenails, corns and calluses, diabetic neuropathy (nerve damage), arthritis, and acquired deformities such as hammertoes and bunions.
Arch pain can be caused by an injury, flat feet, high arches, plantar fasciitis, weight gain, aging, or overuse. It can also be the result of gait abnormalities such as overpronation—where the foot rolls excessively inward causing undue pressure on the arch.
Heel pain is usually attributed to plantar fasciitis, but may also be due to Achilles tendinitis, heel bursitis, Sever’s disease, heel spurs, obesity, poorly fitting shoes, heel pad atrophy, stress fractures or contusions, or arthritis.
Ball of the foot pain occurs in the padding underneath the toes. It can be due to metatarsalgia, metatarsal joint pain, arthritis, plantar warts, stress fractures, obesity, or conditions such as Morton’s neuroma, Freiberg’s disease, or sesamoiditis.
It is important to note that foot pain is not normal, and it should not be ignored. Most conditions that cause foot pain can be treated simply and conservatively, especially when diagnosed and treated early on.
What Podiatrists Can Do for Foot Pain
A podiatrist is a physician that specializes in foot and ankle health. Many are podiatric surgeons as well. Podiatrists are experts at getting to the root cause of foot pain and creating a treatment plan to take care of the condition effectively and promptly.
They can also offer professional advice and tools to help avoid foot pain by:
• Prescribing custom orthotic devices
• Recommending appropriate footwear
• Sharing tips on proper training techniques
• Providing basic care suggestions for maintaining healthy feet.
If you have any foot pain, discomfort, swelling, or decreased immobility, see a podiatrist right away to have your condition diagnosed and treated properly.
